 |
 |
- Search
AbstractObjectivesTo investigate the common causes of persistent septal deviation in revision septoplasty and to report the surgical techniques and results to correct them.
MethodsA total of 100 consecutive patients (86 males) who had revision septoplasty due to persistent septal deviation from 2008 and 2014 were included in the study. Their mean age was 35.6 years and the mean follow-up duration was 9.1 months. Presenting symptoms, sites of persistent septal deviation, techniques used to correct the deviation, and surgical results were reviewed.
ResultsThe mean interval between primary and revision surgery was 6.2 years. Forty-eight patients received revision septoplasty and 52 received revision septoplasty combined with rhinoplasty. Nasal obstruction was the most presenting symptom in almost all patients. The most common site of persistent septal deviation was middle septum (58%) followed by caudal septum (31%). Correcting techniques included further chondrotomy and excision of deviated portion in 76% and caudal batten graft in 39%. Rhinoscopic and endoscopic exams showed straight septum in 97% and 92 patients had subjective symptom improvement postoperatively.
Septoplasty is one of the most commonly performed otolaryngologic procedures to relieve nasal obstruction [1]. However, the success rate of primary septoplasty varies from 43% to 85% [2-5] indicating more than 15% of septoplasty patients fail to relieve their symptom. Persistent nasal obstruction after septoplasty can be attributed to several reasons: residual septal deviation, recurrence of septal deviation, unrecognized nasal valve compromise, improper management of turbinate hypertrophy, or progression of allergic mucosal disease. There are a few reports on the reasons for septoplasty failure and many of them stressed the importance of missed valve problems [6,7]. Among the causes of septoplasty failure, residual or recurred septal deviation due to incomplete or improper correction of the deformity comprises a big part. The purpose of this study is to investigate the common etiologies of failed septal correction after primary septoplasty and to report the surgical techniques to correct them and outcome.
Consecutive 100 patients who underwent revision septoplasty from 2008 to 2014 at the Department of Otorhinolaryngology-Head and Neck Surgery of SMG-SNU Boramae Medical Center were included in the study. All patients had primary septoplasty at other hospital and referred for persistent nasal obstruction. They were screened for other etiologies for recurrent nasal obstruction and had confirmed persistent septal deviation as the main cause of the patient’s presenting symptoms. Demographic data, presenting symptoms, findings of the septum and nasal cavity, time interval between the primary and revision septoplasty, comorbid rhinologic diseases such as allergic rhinitis, chronic sinusitis, and history of facial trauma were evaluated by retrospective chart review. The graphic operation records and medical charts were reviewed to investigate surgical approach, sites of persistent septal deviation, techniques to correct the deviation, combined procedures, surgical results and complications. The Institutional Review Board of Boramae Medical Center permitted this study (IRB No. 20170810/10-2017-22/091).
The sites of persistent septal deviation were categorized into four anatomical areas: caudal septum (caudal end of cartilaginous septum), anterior septum (cartilaginous septum except caudal septum), middle septum (septum around the bony-cartilaginous junction including cartilaginous and bony septum), and posterior septum (bony septum) (Fig. 1).
Status of the septum after surgery was checked with anterior rhinoscopic and endoscopic examination at the last follow-up. They were classified into three categories: straight, improved but with residual deviation remained, and same or worse. Acoustic rhinometry was used in limited patients to evaluate pre- and postoperative nasal cavity volume and cross sectional area. Subjective symptom improvement was assessed at the outpatient clinic and categorized as no improvement (0), slight improvement (1), moderate improvement (2), and much improvement or no obstruction at all (3). Several patients with missing data (scaled comment on subjective symptom improvement) were telephone surveyed separately.
A total 100 patients were enrolled in this study. Eighty-six patients were male and 14 patients were female. The mean age of subjects was 35.6 years (range, 19 to 63 years), and the mean follow-up duration was 9.1 months (range, 3 to 36 months). The mean interval between the primary and revision surgery was 6.2 years and 14 patients had revision in less than 1 year. Forty-eight patients received revision septoplasty and 52 patients received revision septoplasty with combined rhinoplasty. Among 52 rhinoplasty cases, 12 patients had rhinoplasty to correct deformities caused by previous septoplasty (e.g., saddle nose) and remaining 40 patients had rhinoplasty (e.g., radix augmentation or tip-plasty) for additional aesthetic purposes. Endonasal approach was used in 36 patients (36.0%) and open approach was used in 64 patients (64.0%). Forty-six patients received primary septal surgery at private clinics and 54 patients at other general hospitals.
Ninety-six patients presented nasal obstruction as their primary cause for revision surgery. Twelve patients had aesthetic dissatisfaction which included saddle nose in eleven patients and tip ptosis in one patient. Seven patients had septal perforation and five patients had postoperative synechia.
The main sites of persistent septal deviation were middle septum (the most deviated portion at the bony-cartilaginous junction) in 58%, caudal septum in 31%, anterior septum (mostly extending from the dorsal strut) in 21%, and posterior septum in 1% (Table 1). There was no difference in the sites of persistent septal deviation between the patients who had their initial surgery at local clinics and at general hospitals.
In 76 patients, further chondrotomy was done and careful excision of the deviated portion was performed. The caudal batten graft was applied in 39 patients, the spreader graft in 22, the suture fixation of the caudal septum to anterior nasal spine in 17, cutting of cartilage at the most curved portion and realigning with sutures in 11, and partial septal replacement in six (Table 2). Combined surgery included rhinoplasty (n=52), inferior turbinoplasty (n=36), endoscopic sinus surgery (n=9), septal perforation repair (n=7), and synechiolysis (n=5) (Table 3).
Postoperative anterior rhinoscopy and endoscopy showed that a straight septum was achieved in 97 patients but three patients had mild caudal deviation even though much improvement was achieved compared with the preoperative status. No patients had septal deviation that remained unchanged or became worse after surgery.
Both pre- and postoperative acoustic rhinometry was achieved in 16 patients. A statistically significant improvement in the minimal cross-sectional area, from 0.38 cm2 to 0.51 cm2, was achieved in the convex side of the nasal cavity (P=0.003). The minimal cross-sectional area in the concave side of the nasal cavity decreased from 0.51 cm2 to 0.49 cm2, which was not statistically significant (P=0.589). The nasal volume increased in the convex side of the nasal cavity (5.96 mL vs. 7.26 mL), and the nasal volume of the concave side decreased after surgery (7.71 mL vs. 6.36 mL), but both differences were not statistically significant (P=0.071 and P=0.055).
After surgery, 65 patients had much improvement in nasal obstruction, 21 patients had moderate improvement, and six patients had slight improvement. But eight patients had recurred obstruction or no improvement at all. Among 14 patients who had less than moderate improvement, the most common reason for dissatisfaction was uncontrolled allergic rhinitis (n=9), residual septal deviation (n=3), recurrent sinusitis (n=3), and remained septal perforation (n=2). Among three patients with residual septal deviation, one patient who developed mild deviation of the caudal septum and synechia, underwent secondary revision septoplasty with synechiolysis and the symptom improved.
In previous studies, recurrent nasal obstruction after primary septoplasty was attributed to the residual or recurrent septal deviation, missed nasal valve collapse, turbinate problem, or untreated allergic rhinitis. The proportions of these causes may differ depending on the surgeon, country, or race. For example, residual septal deviation can be more prevalent in beginners and recurrent contralateral deviation can occur by improper correction in more aggressive surgeons. Race can also influence the results because Asians have weak, small cartilaginous septum while they have less valve problems than Caucasian nose.
The prevalent sites of persistent septal deviation in failed septoplasty were not frequently addressed [2,7-9]. A few studies reported that the common sites of residual deviation are dorsal or caudal septum. Becker et al. [7] reported that multiple (caudal and dorsal) sites of deviation was the most common (48%) in revision cases, and caudal septal deviation was the second (28%). Other study reported that residual septal deviation was at the caudal septum (36%), and dorsal septum (28%) in order [2]. In this study, we divided septum into caudal, anterior, middle, and posterior septum. Compared to several classifications in previous studies, this classification collectively covers the whole septum. Also, the classification areas were named according to their relative position in the septum for easy reading and communication. We did not include dorsal septum as a separate site in this study because remaining deviation of the dorsal strut alone is not frequent. Dorsal strut area can be upper part of anterior septum, and its deviation is usually combined with deviation of the remaining lower part of anterior septum or caudal septum.
Our study shows the most prevalent site of persistent septal deviation is middle septum, with the most deviated portion at the bony-cartilaginous junction. Because many septal deviations are general concavity and convexity where the center is located at bony-cartilaginous junction, persistent deviation in this place means proper and sufficient chondrotomy was not done at the primary surgery.
In this study, when there was persistent middle septal deviation, further chondrotomy and conservative excision of deviated portion usually corrected the residual deviation (Fig. 2). Unskillful surgeons have a tendency not to separate bony-cartilaginous junction high enough to sufficiently remove the external deviating force of the ethmoid plate because they are afraid of injuring the keystone area, which may lead to inverted V deformity. In fact, there were cases that even the bony-cartilaginous junction was not separated and only cross-hatching incision at the cartilaginous septum was present. This timid chondrotomy somewhat indicates the skill level of the first surgeon. Too much emphasis on the preservation of the keystone area hinders proper chondrotomy that may cause this problem.
Consistent with previous studies, the caudal septum was also a major site of persistent deviation. There can be three scenarios when caudal septum is still deviated after septoplasty: first, the deviation was not corrected at all. Second, the deviation was not fully addressed, thus ended up with incomplete correction. Third, redeviation was in the other direction after initial proper correction. In our series, many of the patients had no evidence of attempted procedures to correct it. Because of the importance of the support provided by the caudal septum, the structural integrity of the caudal septum must not be compromised by incisions or excisions and should be reconstructed after manipulations. Weakening of caudal septum and separation with anterior nasal spine commonly result in saddle deformity or tip ptosis, so many surgeons hesitate to correct caudal deviation perfectly and some of them even do not touch it.
Some of the patients had cross-hatching incisions of the cartilaginous septum (Fig. 3), which is a sign of failed attempt to correct the deviation at the primary surgery. Most of the hatching incisions were not full in depth, thus not reaching the contralateral perichondrium of the septum. Some of them had full depth of incision but failed to correct the deviation without any batten graft. Cross-hatching incision has been accepted as one of the methods until recently to correct the residual cartilaginous deviation after chondrotomy [10]. However, this cross-hatching incision technique is thought to be overemphasized and is rarely used nowadays. Several studies reported that cross-hatching incisions were ineffective for the correction because it did not remove the extrinsic forces that are generated by the neighboring bony structures [11,12]. Other studies reported weakening of the cartilage and overcorrection due to overzealous cross-hatching incisions [6,11-13]. Especially in Asian who has thin, weak septal cartilage, straightening of the septal cartilage with cross-hatching incision without proper battening fails to correct the curvature of the septum or leads to another deformity.
Authors used batten graft to correct caudal septum deviation when it became too weak or unstable after proper correction (Fig. 4). In this study, batten graft was used in 39 cases and they all had good results. Batten graft has been introduced for correction of caudal deviation to prevent the occurrence of subsequent nasal deformities due to the weakening of the caudal septal support [14-16]. Especially in revision surgery, batten graft is often needed to support caudal septum, which has been weakened and crumbled by previous excision. With strong caudal septal support, septum straightening with proper dorsal support is possible.
Half of our patients had concurrent rhinoplasty with septoplasty. These include patients who wanted aesthetic nasal improvement together with septal correction, patients who needed open septorhinoplasty to correct the difficult-to-correct dorsal deviation at caudal or anterior septum, and patients who needed concurrent septal perforation repair with rhinoplasty. High septal deviation reaching dorsum often needs separation of upper lateral cartilage and the septum with techniques to correct the deformity such as spreader/batten graft, cutting of curved dorsal septum with realignment, or subtotal/total reconstruction. Although these techniques can be done endonasally, they are facilitated with open approach.
The subjective symptom improvement and objective rhinoscopy findings indicate effectiveness of the revision septoplasty techniques that we used. Among 14 patients who did not gain significant symptom improvement, nine patients got controlled after proper allergy medication. Among three patients who had persistent septal deviation, one patient with synechia underwent secondary revision septoplasty with synechiolysis. Postoperatively, the patient’s symptom was much improved subjectively and his septum became straight.
In conclusion, we found that incomplete separation and resection of bony-cartilaginous junction and inadequate correction of the caudal septal deviation are the main reasons for persistent septal deviation after primary septoplasty. These problems can be solved by proper chondrotomy with conservative excision of deviated septum, and correction of the caudal deviation with batten graft.
▪ Septoplasty is one of the most commonly performed otolaryngologic procedures, but more than 15% of septoplasty patients fail to relieve their symptom.
▪ Incomplete separation and resection of bony-cartilaginous junction and inadequate correction of the caudal septal deviation are the main reasons for persistent septal deviation after primary septoplasty.
▪ It can be solved by proper chondrotomy with conservative excision of deviated septum, and correction of the caudal deviation with batten graft.
Fig. 1.Dividing the septum into four areas. a: Caudal septum (caudal end of cartilaginous septum), b: anterior septum (cartilaginous septum except caudal septum), c: middle septum (area around the bony-cartilaginous septum), d: posterior septum (bony septum). 
Fig. 2.Persistent curved deformity after septoplasty and more chondrotomy to relieve deforming forces of the bony septum. (A) Persistent curvature of the septal cartilage is observed after full exposure of the septum after separation from the upper lateral cartilages. (B) Further chondrotomy was done for correction. Partial hatching incision attempted at previous surgery is also observed at the inferior portion of the caudal septum. 
Fig. 3.Cross-hatching incisions performed on the concave side of septal cartilage at previous surgery are observed. Some of the incisions were too deep and some of them were too superficial and failed to correct the curvature of the septal cartilage. 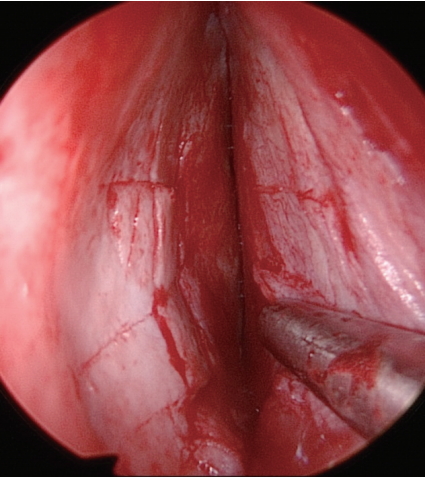
Fig. 4.Batten graft with septal bone to correct caudal septal deformity. (A) Open approach. (B) Endonasal approach. 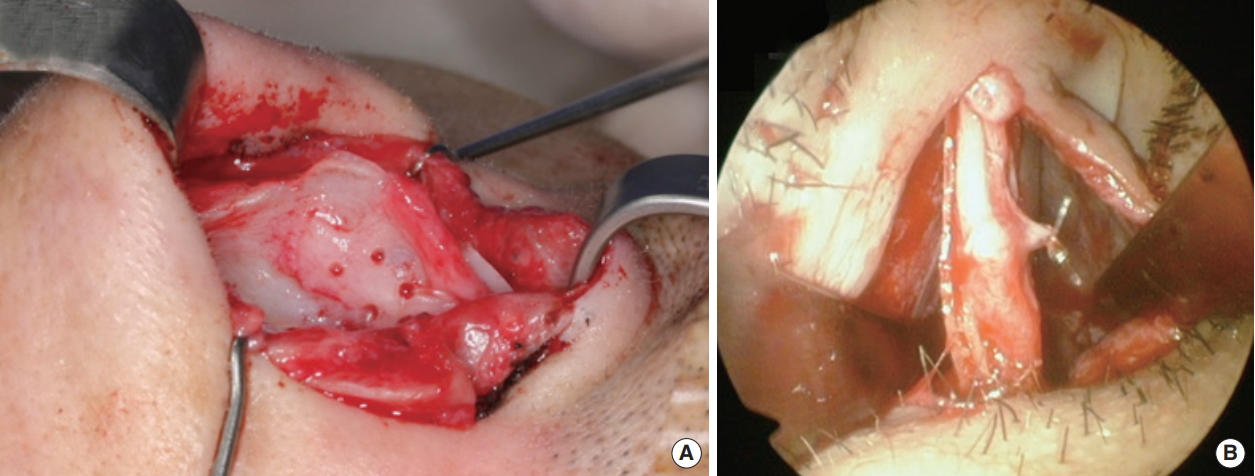
Table 1.Sites of persistent septal deviation (n=100)
Table 2.Main operative procedures to correct persistent septal deviation (n=100)
Table 3.Combined surgery with revision septoplasty (n=100)
REFERENCES1. Uppal S, Mistry H, Nadig S, Back G, Coatesworth A. Evaluation of patient benefit from nasal septal surgery for nasal obstruction. Auris Nasus Larynx. 2005 Jun;32(2):129-37.
2. Gillman GS, Egloff AM, Rivera-Serrano CM. Revision septoplasty: a prospective disease-specific outcome study. Laryngoscope. 2014 Jun;124(6):1290-5.
3. Siegel NS, Gliklich RE, Taghizadeh F, Chang Y. Outcomes of septoplasty. Otolaryngol Head Neck Surg. 2000 Feb;122(2):228-32.
4. Illum P. Septoplasty and compensatory inferior turbinate hypertrophy: long-term results after randomized turbinoplasty. Eur Arch Otorhinolaryngol. 1997 Jan;254 Suppl 1:S89-92.
5. Fjermedal O, Saunte C, Pedersen S. Septoplasty and/or submucous resection? 5 Years nasal septum operations. J Laryngol Otol. 1988 Sep;102(9):796-8.
6. Lee BJ, Chung YS, Jang YJ. Overcorrected septum as a complication of septoplasty. Am J Rhinol. 2004 Nov-Dec;18(6):393-6.
7. Becker SS, Dobratz EJ, Stowell N, Barker D, Park SS. Revision septoplasty: review of sources of persistent nasal obstruction. Am J Rhinol. 2008 Jul-Aug;22(4):440-4.
8. Dinis PB, Haider H. Septoplasty: long-term evaluation of results. Am J Otolaryngol. 2002 Mar-Apr;23(2):85-90.
9. Sedwick JD, Lopez AB, Gajewski BJ, Simons RL. Caudal septoplasty for treatment of septal deviation: aesthetic and functional correction of the nasal base. Arch Facial Plast Surg. 2005 May-Jun;7(3):158-62.
10. Murakami WT, Wong LW, Davidson TM. Applications of the biomechanical behavior of cartilage to nasal septoplastic surgery. Laryngoscope. 1982 Mar;92(3):300-9.
11. Heo SJ, Kim JS. Crosshatching incision technique in septoplasty: experimental outcomes under actual surgical settings. Auris Nasus Larynx. 2016 Oct;43(5):518-23.
12. Ozyazgan I, Idaci O. A new method that uses cyanoacrylate tissue adhesive to fill scoring incisions in septal cartilage correction. Laryngoscope. 2011 Jun;121(6):1164-72.
13. Min YG, Chung JW. Cartilaginous incisions in septoplasty. ORL J Otorhinolaryngol Relat Spec. 1996 Jan-Feb;58(1):51-4.
14. Wee JH, Lee JE, Cho SW, Jin HR. Septal batten graft to correct cartilaginous deformities in endonasal septoplasty. Arch Otolaryngol Head Neck Surg. 2012 May;138(5):457-61.
|
|
|||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||







