 |
 |
- Search
AbstractObjectives. Sigmoid sinus resurfacing (SS-R) is one of the most effective surgical treatments for patients with pulsatile tinnitus (PT) originating from anatomical variants of the vascular walls in the temporal bone. This study aimed to provide updated information on the clinical outcomes of SS-R and evaluate the efficacy of the water occlusion test (WOT) as an additional diagnostic modality.
Methods. We retrospectively reviewed medical records including tinnitus questionnaires, temporal bone computed tomography (TBCT) scans, audiologic tests, and preoperative WOT results from patients who underwent SS-R.
Results. In total, 26 patients were included in the study. The mean age was 44 years, and the mean symptom duration was 3 months. Fourteen patients (53.8%) were completely cured, seven (26.9%) significantly improved, and five (19.2%) remained stable. The mean visual analog scale loudness score decreased from 5.26 to 1.34 (P<0.001) and the mean Tinnitus Handicap Inventory score also improved from 50.23 to 5.5 (P<0.001) after SS-R surgery. In 10 patients with discrepancies between the preoperative TBCT and intraoperative findings, WOT showed a significant additive effect in predicting surgical outcomes. No patients experienced severe intraoperative or postoperative complications during the entire follow-up period.
Conclusion. SS-R provides significant symptom improvement in patients with sigmoid sinus dehiscence who had a positive WOT without other sigmoid sinus variants. A combined diagnostic approach with TBCT, WOT, and intraoperative findings is crucial for achieving better surgical outcomes in patients with PT caused by sigmoid sinus variants.
Tinnitus refers to the perception of sound in the absence of any external auditory stimulus. It can be divided into two categories: subjective and objective tinnitus. Objective tinnitus is further classified into vascular and non-vascular tinnitus, based on its origin. Vascular tinnitus, also referred to as pulsatile tinnitus (PT), accounts for about 10% of all tinnitus cases [1]. Up to 92% of PT cases have identifiable underlying causes [2], offering the possibility of symptom relief through surgical intervention. The causes of PT include significant vascular wall abnormalities in the temporal bones [3,4]. There are three potential mechanisms that explain how these anomalies cause PT: (1) turbulence in blood flow due to alterations in vascular hemodynamics [5,6], (2) vibration of a dehiscent vascular wall in the absence of turbulent flow [7,8], and (3) third-window lesions in the inner ear causing abnormal sound perception [9,10]. Among the various vascular wall abnormalities, sigmoid sinus abnormalities are the most common identifiable cause of PT of venous origin, with a prevalence of approximately 20% in PT patients [8,11,12].
An accurate diagnosis of the underlying anatomical abnormality is critically important before proceeding with surgery for the treatment of PT. This can be achieved through a combination of history-taking, physical examination, audiologic tests, laboratory tests, imaging examination, ultrasonography, and the water occlusion test (WOT) [13]. The aim of this study was to analyze the outcomes of surgery for PT and to evaluate the efficacy of the WOT as a powerful additional tool in diagnostic process, when used in conjunction with temporal bone computed tomography (TBCT) to determine the optimal surgical modality for vascular wall anomalies causing PT.
We included patients with PT who visited Seoul St. MaryŌĆÖs hospital between April 2018 and December 2021 and underwent sigmoid sinus resurfacing (SS-R) surgery. All patients were treated with tinnitus retraining therapy, along with medication including anxiolytics and beta blocker, for a minimum of 3 months. Additionally, any potential metabolic or hemodynamic causes such as hypertension, hyperthyroidism, anemia, etc., were corrected if present. Surgical intervention was determined if there was no improvement in symptoms even after 3 months of this conservative treatment. For pre-operative evaluation, TBCT and WOT were performed to obtain information about anatomical variations and to plan appropriate surgical methods. Tinnitus visual analog scale (VAS), loudness (LD), awareness (AW), annoyance (AN), effect on life (EF), and Tinnitus Handicap Inventory (THI) scores from a tinnitus questionnaire were used for comparing subjective outcomes, and pure tone audiograms were also compared for objective pre- and postoperative outcomes. VAS LD score and THI score were analyzed for primary and secondary outcomes, respectively. Surgical outcomes were classified into four groups according to VAS LD; complete cure when reduction of VAS LD is 100%, significant improvement when between 50%ŌĆō99%, stationary status when between 1% and 49%, and no improvement when at 0% [4,14].
This study was approved by the Institutional Review Board of the Clinical Research Institute at Seoul St. MaryŌĆÖs Hospital (No. KC21RASI0524) and was conducted in accordance with the Declaration of Helsinki. Informed consent requirement was waived.
After positioning the patientŌĆÖs head tilting to the healthy side by about 10┬░, we filled the external auditory canal (EAC) of the PT side with a few milliliters of sterilized normal saline solution at body temperature under microscopy. Any changes in tinnitus symptoms were requested from the patients and results of the WOT were classified as positive when PT fully ceased, partial when PT decreased but is still present, and negative when PT shows no change or is worsened by the test [13].
SS-R surgery for sigmoid sinus dehiscence (SS-Deh) was conducted using the following steps: (1) simple cortical mastoidectomy, (2) skeletonizing the SS and exposure of the dehiscent area by removing the mucosa, and (3) resurfacing and reinforcing the SS wall using an autologous bone pate and bone cement (Fig. 1A). Other surgical techniques including SS diverticulum obliteration with a periosteal flap (Fig. 1B), jugular bulb resurfacing, or emissary vein ligation (Fig. 1C) were performed in addition to SS-R based on the diagnosis confirmed by the combination of TBCT, WOT, and intraoperative findings.
The total number of enrolled patients was 26 (7 men, 19 women), and their mean age was 44┬▒13.8 years (range, 18ŌĆō75 years). The mean symptom duration was 30.8┬▒39.4 months. Of the 26 patients, 21 had right-side tinnitus and five had left-side tinnitus. Sixteen patients showed positive results on the WOT. Seven patients showed a partial response, and three patients showed negative results on the WOT.
Preoperative TBCT scans demonstrated SS-Deh in 23 cases (Fig. 2A), sigmoid sinus diverticulum (SS-Div) in seven cases (Fig. 2B), dehiscent high riding jugular bulb (HJB-Deh) in three cases, and six cases of prominent mastoid emissary vein (PMEV) (Fig. 2C). The mean postoperative follow-up duration was 13.2┬▒8.3 months. Every patient underwent SS-R surgery, along with additional surgery according to the final PT diagnosis and WOT results. PatientsŌĆÖ demographic characteristics and surgical outcomes are summarized in Table 1.
The overall subjective surgical outcomes were as follows: 14 patients (53.8%) experienced a complete cure of tinnitus, 7 patients (26.9%) showed significant improvement, 5 patients (19.23%) showed a stable status, and no patients showed no improvement. The mean (┬▒standard deviation [SD]) VAS LD score significantly improved from 5.26┬▒2.03 to 1.34┬▒1.85 (P<0.001, Wilcoxon signed-rank test) and the other VAS scores, presented in Fig. 3A, also showed significant improvements after SS-R with or without accompanying surgery (P<0.001, Wilcoxon signed-rank test) (Fig. 3A and B). The mean (┬▒SD) THI score also improved from 50.23┬▒23.68 to 5.5┬▒12.74 (P<0.001, Wilcoxon signed-rank test) (Fig. 3C and D).
Upon pure-tone audiograms, 13 patients showed pseudo-low frequency hearing loss (an ipsilateral hearing threshold greater than 10 dB HL at both 250 and 500 Hz, or greater than 20 dB HL at either 250 or 500 Hz compared with the contralateral side) [15] in the ipsilesional ear, and the hearing threshold improved in 12 patients. Ten patients exhibited discrepancies between the preoperative TBCT and intraoperative findings. Specifically, eight cases of SS-Deh were in actuality cases of thin SS plate, three cases of PMEV were not prominent in the mastoid cavity, and one case of SS-Div was not an actual diverticulum. Among these 10 patients, nine patients achieved successful surgical outcomes based on the WOT results. Even though the intraoperative findings showed a thin SS plate, when SS-R was performed according to positive WOT results, four patients experienced complete resolution and two showed significant improvement. One patient who underwent SS-R despite negative WOT results demonstrated stable outcomes. Another patient, whose surgical findings revealed a thin SS plate with SS-Div, was treated with SS-R and SS-Div obliteration using a periosteal flap [16], in accordance with negative WOT results, and showed complete resolution. Finally, one complete resolution and one significant improvement were achieved when SS-R was performed based on positive WOT results in two patients. In these cases, PMEV was detected only on TBCT and was not specifically addressed intraoperatively.
Interestingly, the cure rate for SS-R surgery in patients suffering from PT, caused solely by SS-Deh, was as high as 66.7%. This was observed in patients who demonstrated positive TBCT and intraoperative findings, along with a positive WOT. The remaining patients also exhibited significant improvement. This suggests that the combined approach of TBCT, WOT, and intraoperative findings holds excellent prognostic value for the surgical outcomes of SS-R. Postoperatively, there were no complications except for one case (no. 13 in Table 1) of newly developed mild conductive hearing loss (Fig. 4).
In this study, we observed a high success rate of SS-R in patients with PT originating from sigmoid sinus variants. Of the 26 patients enrolled in the study, 21 (80.76%) showed a significant improvement in symptoms post-surgery. Additionally, the study aimed to validate the prognostic value of the WOT, a method previously published by our research group [13], by analyzing the surgical outcomes of SS-R in PT patients based on the WOT results. However, five patients exhibited no change in surgical outcomes, despite preoperative diagnosis using TBCT, intraoperative findings, and the WOT. The first patient (no. 6 in Table 1), who had preoperative TBCT and intraoperative findings of SS-Deh and SS-Div underwent SS-R alone, which resulted in no change in outcome. In this patient, the WOT result was partial, suggesting that her SS-Div significantly impacted her PT symptoms. Therefore, reshaping the sigmoid sinus to reduce turbulence in the SS-Div or obliterating it with a periosteal flap might be necessary to achieve successful surgical outcomes. As previously reported, partial results in the WOT, which support the impact of SS-Div on symptoms, occur because water occlusion of the EAC only reduces sound coming from the venous sinus dehiscence but does not affect, or even amplifies, turbulence sounds originating from SS-Div, PMEV, or an arteriovenous fistula [13]. In more detail, pulsatile sound from the venous sinus dehiscent site is transmitted to the tympanic membrane through air transmission (air pulsation mechanism), while pulsatile sound from turbulent blood flow can be directly transmitted to the cochlea through bone conduction (turbulence conduction mechanism). Given that water occlusion of the EAC only affects the movement of the tympanic membrane, SS-Deh and HJB-Deh may show positive results in the WOT, whereas SS-Div, PMEV, and arteriovenous fistula may show partial or negative results in the WOT.
The mastoid emissary vein (MEV) is a normal venous structure connecting the extracranial venous system and sigmoid sinus [17] that is found in the majority of the population and typically has no significant clinical features [18]. Kim et al. [19] reported that the prevalence of MEV was 74% on the left side and 81% on the right side, and the mean mastoid emissary foramen diameter was 1.73 mm. Forte et al. [20] measured the internal foramina of sigmoid sinuses in 50 normal cadaver skulls and reported that 60% had diameters smaller than 2 mm and 85% had diameters smaller than 3.5 mm [18]. Although most MEVs do not display significant clinical features, those with a diameter large enough to cause turbulence could potentially contribute to PT. In our study, TBCT revealed six cases of PMEV, with a mean diameter of 2.72 mm. Among them, two patients (no. 15 and 16 in Table 1) had only PMEV contributing to PT, with diameters of 2.59 mm and 2.4 mm respectively, and their WOT results were both partial. One patient underwent only SS-R and the other underwent SS-R with emissary vein ligation surgery. Their surgical outcomes were both stable; however, their THI scores varied, with one increasing by 100% and the other decreasing by 97%. Based on this intriguing result, we suggest that a confirmed diagnosis of PMEV, obtained through various diagnostic tools including the WOT, should be managed with emissary vein ligation surgery to alleviate symptoms.
One patient (No. 13 in Table 1), who showed SS-Deh, HJB-Deh, and PMEV on TBCT preoperatively, was confirmed to have a thin SS plate and HJB-Deh intraoperatively. Based on the positive WOT results in this patient, only SS-R and HJB-R were performed. The surgical outcome was stable, with a reduction of 14.2% in VAS LD and 58.2% in THI. However, the evaluation of the surgical outcome in this patient was limited due to the onset of mild conductive hearing loss post-surgery, likely caused by a minor disturbance of air conduction associated with the resurfacing materials. The final patient (no. 26 in Table 1), who exhibited SS-Deh in preoperative TBCT and was found to have a thin SS plate during surgery, demonstrated negative WOT results. The unchanging outcome of the surgery in this patient underscores the clinical prognostic value and significance of WOT once more.
Based on an analysis of 10 cases that showed discrepancies between preoperative TBCT and intraoperative surgical findings, as well as five cases with consistent results, we acknowledge the limitations of using TBCT and intraoperative findings to diagnose anatomical abnormalities. This is particularly relevant when predicting the surgical outcomes of PT. Therefore, we propose that a comprehensive diagnostic evaluation for PT, which includes preoperative TBCT, WOT, and intraoperative findings, may be essential in identifying the best surgical approaches and ensuring successful surgical results. Although the prior report primarily highlighted the diagnostic significance of a new WOT based on potential PT mechanisms [13], our study aims to underscore the importance of WOT in deciding surgical procedures, in conjunction with surgical findings and outcomes.
Our study has certain limitations that should be acknowledged and addressed in future research. Firstly, our study was retrospective in nature, with a relatively small sample size, and all surgeries were conducted by a single surgeon at one institution. Future research should be prospective, encompassing a larger sample size, and should include data from SS-R operations performed by multiple surgeons across various hospitals, all using the same method. Secondly, we only analyzed subjective outcomes when evaluating the surgical results in this study. Objective outcomes, such as those provided by Lee et al. [21] should be considered in the analysis of PT. Finally, the evaluation of the surgical management efficacy of PMEV in this study may have been limited due to the inclusion of only one patient. To evaluate surgical outcomes, we need data from a larger number of patients with PMEV causing PT who have undergone emissary vein ligation surgery.
NotesAUTHOR CONTRIBUTIONS Conceptualization: SNP, JHL, JSH. Data curation: JHL, JSH, AA. Investigation: JHL, JSH, JHS, SYP, SNP. Methodology: JHL, JSH, AA, JHS, SYP, SNP. Project administration: SNP, JHL, JSH. Software: JHL, JSH. Supervision: JHS, SYP, SNP. Validation: SNP, JHL, JSH. Visualization: SNP, JHL, JSH. WritingŌĆōoriginal draft: JHL, JSH. WritingŌĆōreview & editing: all authors. ACKNOWLEDGMENTSThis research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (2021R1F1A1049965).
The authors would like to thank Ms. Hyo Jeong Yang for the medical illustrations describing the sigmoid sinus resurfacing surgery.
Fig.┬Ā1.Multiple surgical methods for the treatment of pulsatile tinnitus. (A) Sigmoid sinus resurfacing surgery (SS-R) with autologous bone plate and bone cement for the treatment of sigmoid sinus dehiscence. (B) Obliteration with an inferiorly based periosteal flap for the treatment of sigmoid sinus diverticulum. (C) Ligation of the vein for the treatment of a prominent mastoid emissary vein. 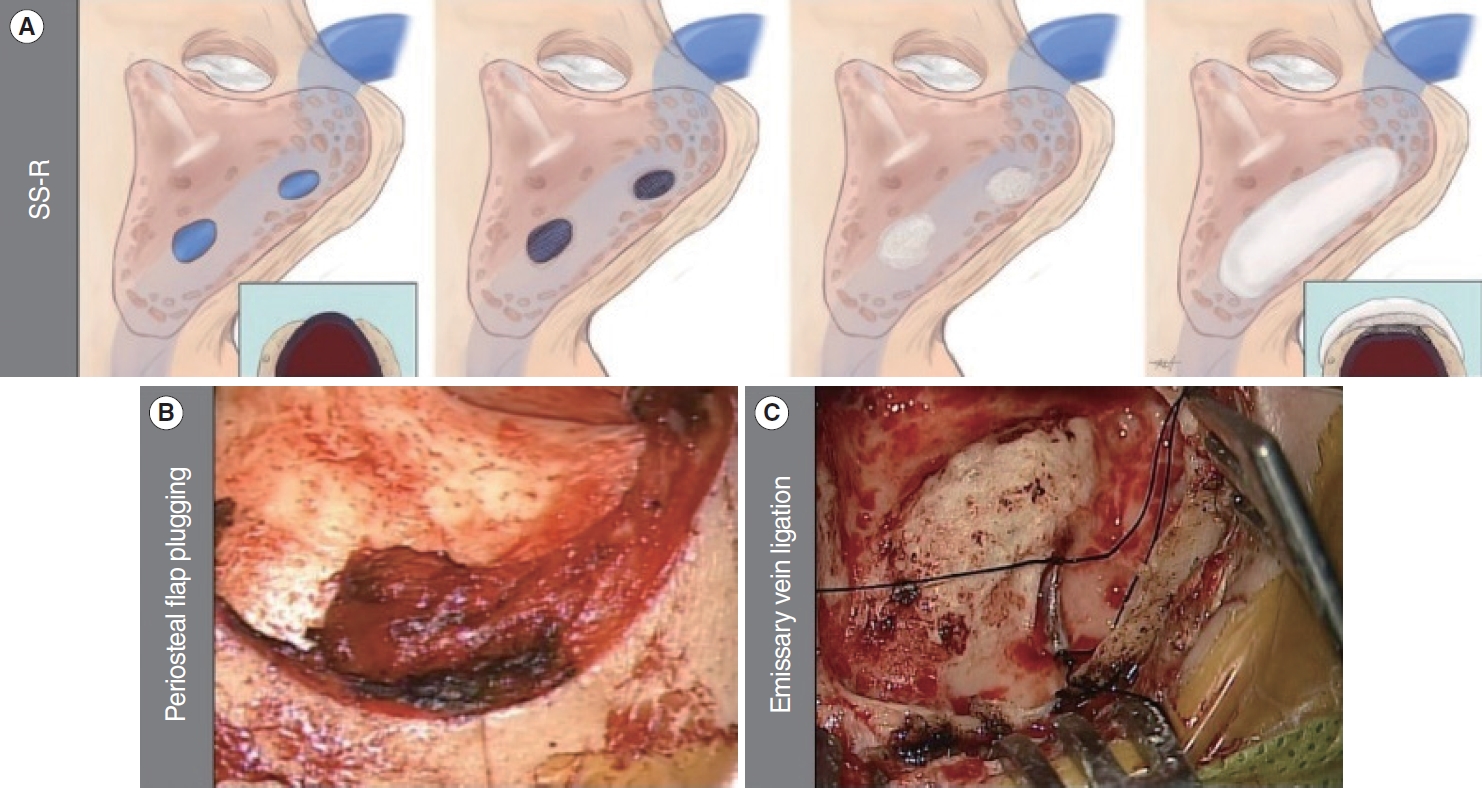
Fig.┬Ā2.Representative axial temporal bone computed tomography images of the right temporal bone showing various causes of pulsatile tinnitus. (A) Sigmoid sinus dehiscence (SS-Deh; arrow). (B) Sigmoid sinus diverticulum (SS-Div; arrows). (C) Prominent mastoid emissary vein (PMEV; arrow). 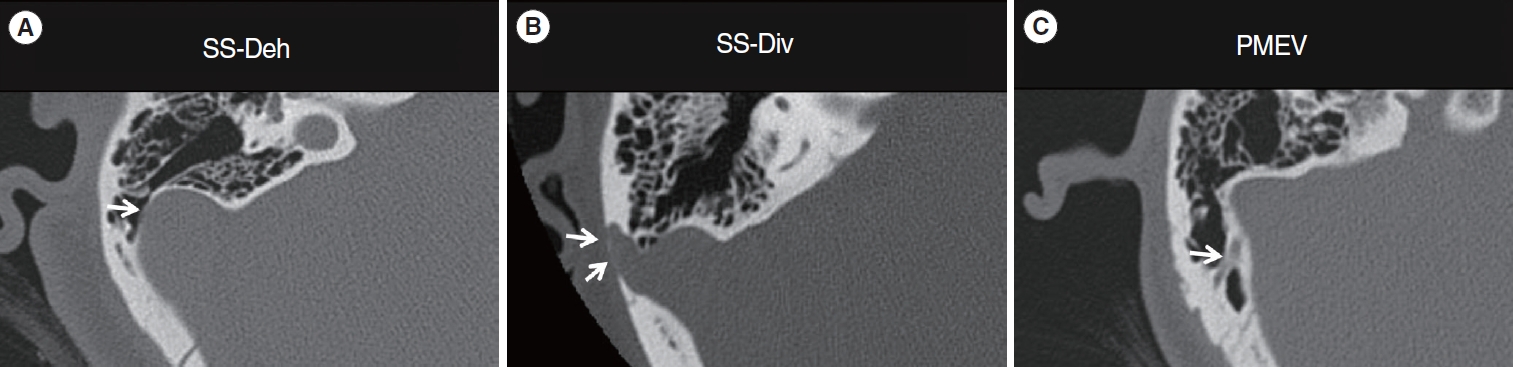
Fig.┬Ā3.Surgical outcomes. (A) Preoperative and postoperative improvements in visual analog scale (VAS) scores. (B) Preoperative and postoperative changes in VAS loudness scores. (C) Preoperative and postoperative improvements in Tinnitus Handicap Inventory (THI) scores. (D) Preoperative and postoperative changes in THI scores. Values are presented as mean┬▒standard deviation. 
Fig.┬Ā4.(A) Preoperative and (B) postoperative pure tone audiograms of a patient managed with sigmoid sinus resurfacing and high-jugular bulb resurfacing who showed newly developed conductive hearing loss as a complication of surgery. 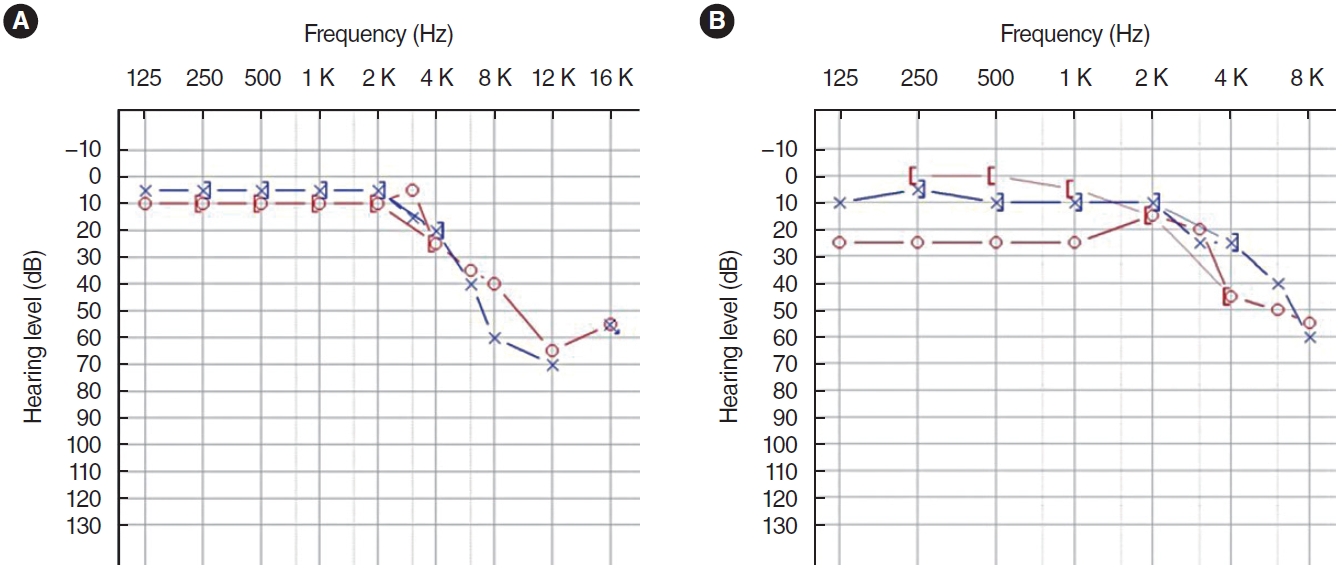
Table┬Ā1.Clinical features and demographic data of 26 patients TBCT, temporal bone computed tomography; MEV, mastoid emissary vein; LD, visual analog scale loudness score; THI, Tinnitus Handicap Inventory; Rt, right; Lt, left; SS-Deh, sigmoid sinus dehiscence; SS-Div, sigmoid sinus diverticulum; SS-R, sigmoid sinus resurfacing surgery; HJB-Deh, dehiscent high riding jugular bulb; PMEV, prominent mastoid emissary vein; JB-R, jugular bulb resurfacing surgery; Div-obliteration, diverticulum obliteration surgery; EV ligation, emissary vein ligation surgery. REFERENCES1. Liyanage SH, Singh A, Savundra P, Kalan A. Pulsatile tinnitus. J Laryngol Otol. 2006 Feb;120(2):93-7.
2. Aggarwal R, Lloyd S. Pulsatile tinnitus. Otorhinolaryngology. 2012;5(1):7-14.
3. Kim CS, Kim SY, Choi H, Koo JW, Yoo SY, An GS, et al. Transmastoid reshaping of the sigmoid sinus: preliminary study of a novel surgical method to quiet pulsatile tinnitus of an unrecognized vascular origin. J Neurosurg. 2016 Aug;125(2):441-9.
4. An YH, Han S, Lee M, Rhee J, Kwon OK, Hwang G, et al. Dural arteriovenous fistula masquerading as pulsatile tinnitus: radiologic assessment and clinical implications. Sci Rep. 2016 Nov;6:36601.
5. Sanchez TG, Murao M, de Medeiros IR, Kii M, Bento RF, Caldas JG, et al. A new therapeutic procedure for treatment of objective venous pulsatile tinnitus. Int Tinnitus J. 2002;8(1):54-7.
6. Kao E, Kefayati S, Amans MR, Faraji F, Ballweber M, Halbach V, et al. Flow patterns in the jugular veins of pulsatile tinnitus patients. J Biomech. 2017 Feb;52:61-7.
7. Eisenman DJ. Sinus wall reconstruction for sigmoid sinus diverticulum and dehiscence: a standardized surgical procedure for a range of radiographic findings. Otol Neurotol. 2011 Sep;32(7):1116-9.
8. Mattox DE, Hudgins P. Algorithm for evaluation of pulsatile tinnitus. Acta Otolaryngol. 2008 Apr;128(4):427-31.
9. Friedmann DR, Le BT, Pramanik BK, Lalwani AK. Clinical spectrum of patients with erosion of the inner ear by jugular bulb abnormalities. Laryngoscope. 2010 Feb;120(2):365-72.
10. Wang JR, Parnes LS. Superior semicircular canal dehiscence associated with external, middle, and inner ear abnormalities. Laryngoscope. 2010 Feb;120(2):390-3.
11. Zeng R, Wang GP, Liu ZH, Liang XH, Zhao PF, Wang ZC, et al. Sigmoid sinus wall reconstruction for pulsatile tinnitus caused by sigmoid sinus wall dehiscence: a single-center experience. PLoS One. 2016 Oct;11(10):e0164728.
12. Grewal AK, Kim HY, Comstock RH, Berkowitz F, Kim HJ, Jay AK. Clinical presentation and imaging findings in patients with pulsatile tinnitus and sigmoid sinus diverticulum/dehiscence. Otol Neurotol. 2014 Jan;35(1):16-21.
13. Park SN, Han JS, Park JM, Jin HJ, Joo HA, Park JT, et al. A novel water occlusion test for disorders causing pulsatile tinnitus: our experience in 32 patients. Clin Otolaryngol. 2020 Mar;45(2):280-5.
14. Sunwoo W, Jeon YJ, Bae YJ, Jang JH, Koo JW, Song JJ. Typewriter tinnitus revisited: the typical symptoms and the initial response to carbamazepine are the most reliable diagnostic clues. Sci Rep. 2017 Sep;7(1):10615.
15. Jeon HW, Kim SY, Choi BS, Bae YJ, Koo JW, Song JJ. Pseudo-low frequency hearing loss and its improvement after treatment may be objective signs of significant vascular pathology in patients with pulsatile tinnitus. Otol Neurotol. 2016 Oct;37(9):1344-9.
16. Chua CA, Han JS, Kim Y, Seo JH, Park SN. Silencing pulsatile tinnitus: a novel technique of periosteal flap obliteration for sigmoid sinus diverticulum variants. Otol Neurotol. 2023 Mar;44(3):246-51.
17. San Millan Ruiz D, Gailloud P, Rufenacht DA, Delavelle J, Henry F, Fasel JH. The craniocervical venous system in relation to cerebral venous drainage. AJNR Am J Neuroradiol. 2002 Oct;23(9):1500-8.
18. Louis RG, Loukas M, Wartmann CT, Tubbs RS, Apaydin N, Gupta AA, et al. Clinical anatomy of the mastoid and occipital emissary veins in a large series. Surg Radiol Anat. 2009 Feb;31(2):139-44.
19. Kim LK, Ahn CS, Fernandes AE. Mastoid emissary vein: anatomy and clinical relevance in plastic & reconstructive surgery. J Plast Reconstr Aesthet Surg. 2014 Jun;67(6):775-80.
|
|
|||||||||||||||||||||||||||||||||||||||||||







